Dr. Tatiana Soto
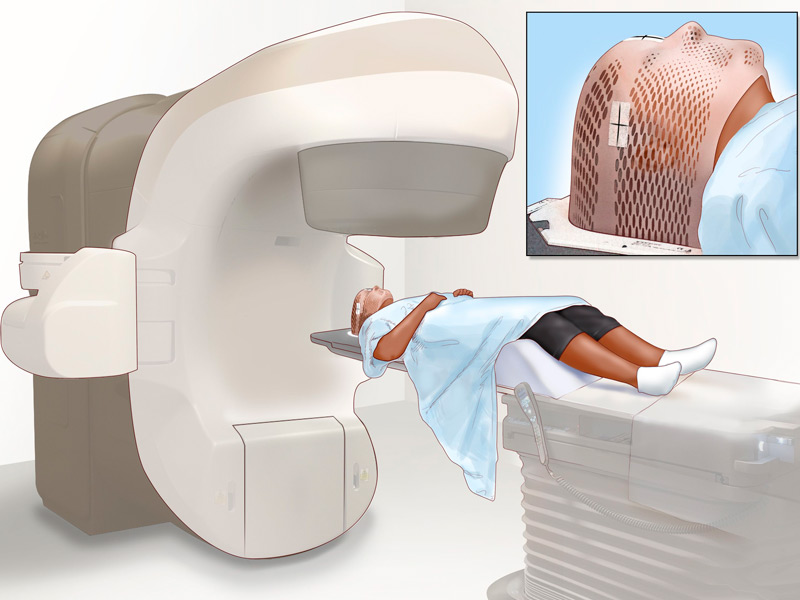
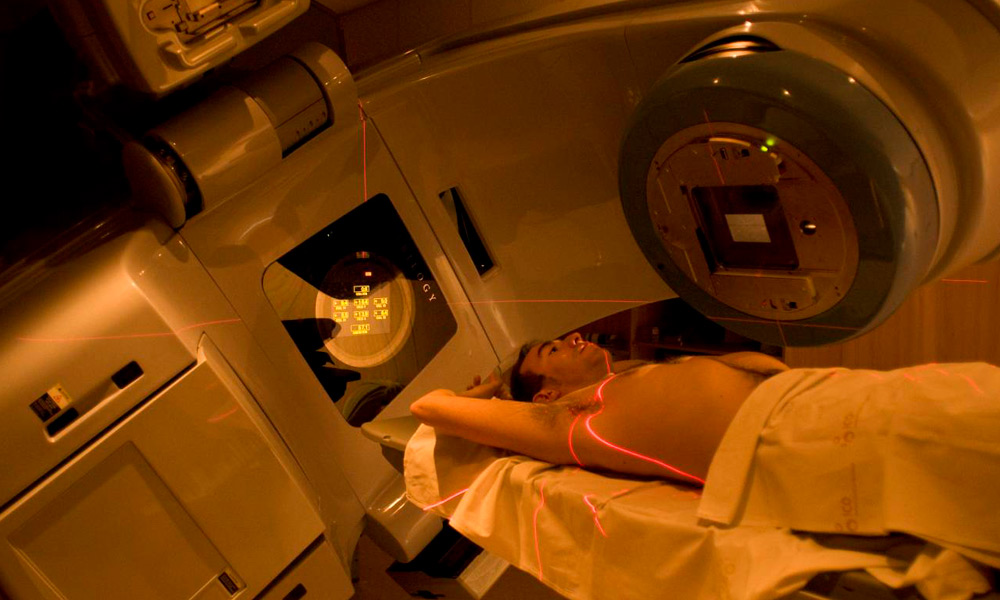
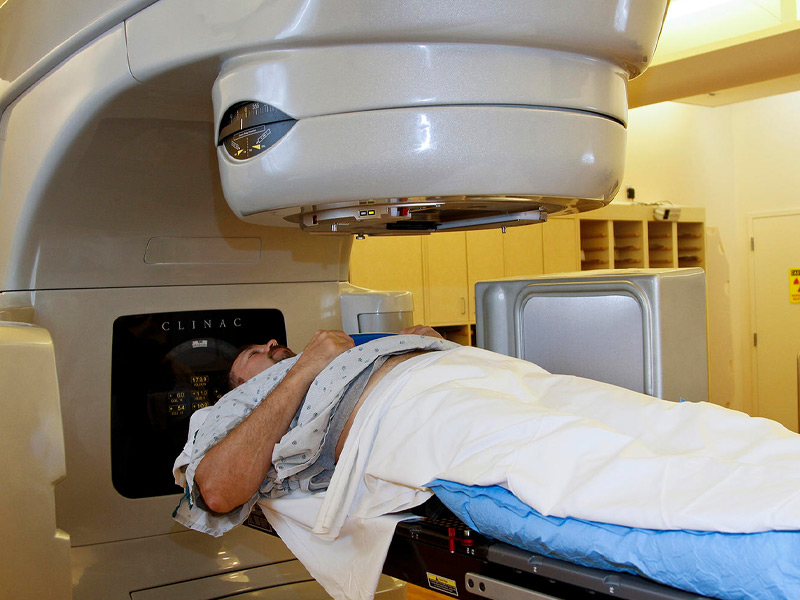
Oncologist and Radiation Therapist
Specialist with extensive experience in radiosurgery treatments. He has knowledge of novel approaches and techniques for intracranial and CNS injuries. Dr. Soto has specialized in comprehensive radiation oncology with an emphasis on short and precise treatments.

Academic education
Doctorate in General Medicine and Surgery
UCIMED University of Medical Sciences | Since 1998
Postgraduate Medical Specialties in Radiotherapy.
University of Costa Rica UCR. | Since 2007
Master's Degree in Health Management.
Central American Institute of Public Administration ICAP | Since 2017
International Master in Advanced Radiotherapy
University of Los Andes, Chile. IAEA-FALP | Since 2018
Work experience
Assistant Physician Specialist in Radiotherapy
San Juan de Dios Hospital | 2011 - Current
Quality Management Committee Coordinator
Radiotherapy Service San Juan de Dios Hospital | 2015 - current
Resident Doctor Specialty Radiotherapy
Calderón Guardia Hospital, Mexico Hospital and San Juan de Dios Hospital | 2007 - 2011
General medicine
National Insurance Institute (INS)
2005 - 2007
General medicine
CARIBBEAN PRESMED